
The two primary types of pulmonary edema include: This fluid buildup can interfere with gas exchange, leading to difficulty breathing and reduced oxygenation of the blood. Pulmonary edema is a condition characterized by the accumulation of fluid in the air spaces (alveoli) and the interstitial space of the lungs. Proper diagnosis and management are vital to address the root cause and prevent complications. Note: While these conditions can cause fluid in the lungs, the clinical presentation, underlying mechanisms, and treatments can vary widely. Toxic Inhalation: Breathing in harmful chemicals or irritants can result in lung injury and subsequent fluid accumulation.Smoke Inhalation: Exposure to significant amounts of smoke, such as in a house fire, can lead to inflammation and fluid buildup.Near Drowning: Inhaling water can cause fluid to accumulate in the lungs.Viral Infections: Some viral infections can lead to fluid buildup in the lungs.Certain Medications: Some drugs, especially certain chemotherapy agents, can cause fluid accumulation in the lungs as a side effect.Lymphatic Obstruction: Conditions like lymphangitis or tumors can block the lymphatic system, causing fluid to build up in the lungs.Lung Injury: Trauma or damage to the lung tissue can result in fluid leakage. 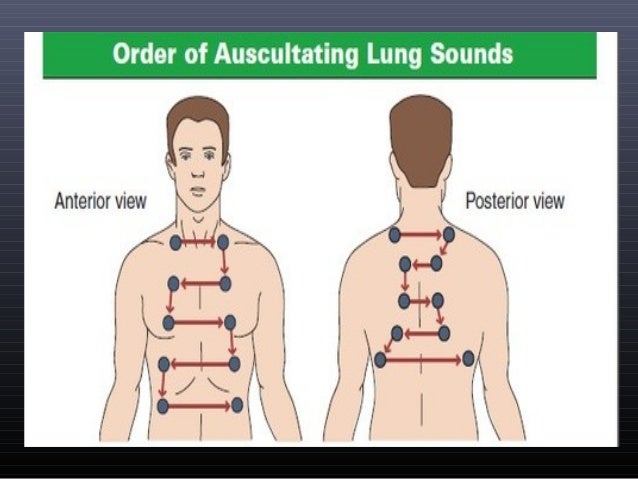
Pulmonary Embolism: A blood clot in the lungs can lead to increased pressure and fluid leakage into the lung tissue.High Altitude Pulmonary Edema (HAPE): This can occur when individuals rapidly ascend to high altitudes, leading to fluid accumulation in the lungs.Severe or chronic kidney disease can lead to fluid buildup, including in the lungs. Kidney Disease: Kidneys play a role in regulating fluid balance in the body.It can compress the lungs and impair respiratory function. Hemothorax: Accumulation of blood in the pleural cavity, typically resulting from chest trauma, surgery, or conditions like pulmonary embolism.Acute Respiratory Distress Syndrome (ARDS): A severe lung condition causing widespread inflammation and fluid buildup in the lungs.Pneumonia: Infection in the lungs can lead to inflammatory responses that cause fluid to accumulate in the alveoli.Congestive Heart Failure (CHF): When the heart is unable to pump blood efficiently, it can lead to a buildup of pressure and fluid leakage into the lungs.Pulmonary Edema: Fluid buildup in the lung’s air spaces and interstitium, often due to heart failure or factors unrelated to heart function, such as infections or toxins.Causes of Fluid in the Lungsįluid accumulation in the lungs can be caused by a variety of conditions, including the following: 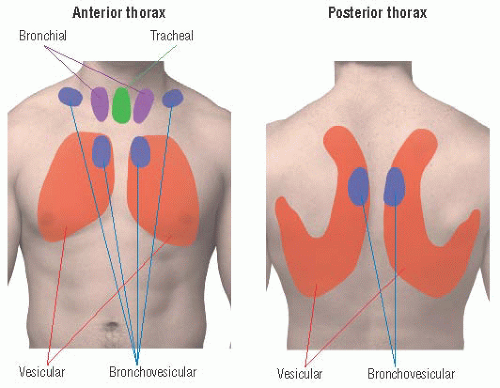
This diagnostic technique allows healthcare professionals to detect and assess abnormalities in organ function, such as heart murmurs or altered lung sounds.Īuscultation is a fundamental component of the physical examination and offers valuable insights into a patient’s health status without the need for invasive procedures or advanced imaging. It is primarily used to assess the functioning of the heart, lungs, and occasionally the gastrointestinal system. Compare both sides symmetrically to distinguish between unilateral or bilateral accumulation, guiding diagnosis and intervention.Īuscultation is the medical practice of listening to the internal sounds of the body using a stethoscope. Listen for characteristic crackles or rales, indicating fluid. When assessing for fluid collection in the lungs during auscultation of lung sounds, you should start at the lower lung fields and determine at which level you start hearing clear breath sounds. 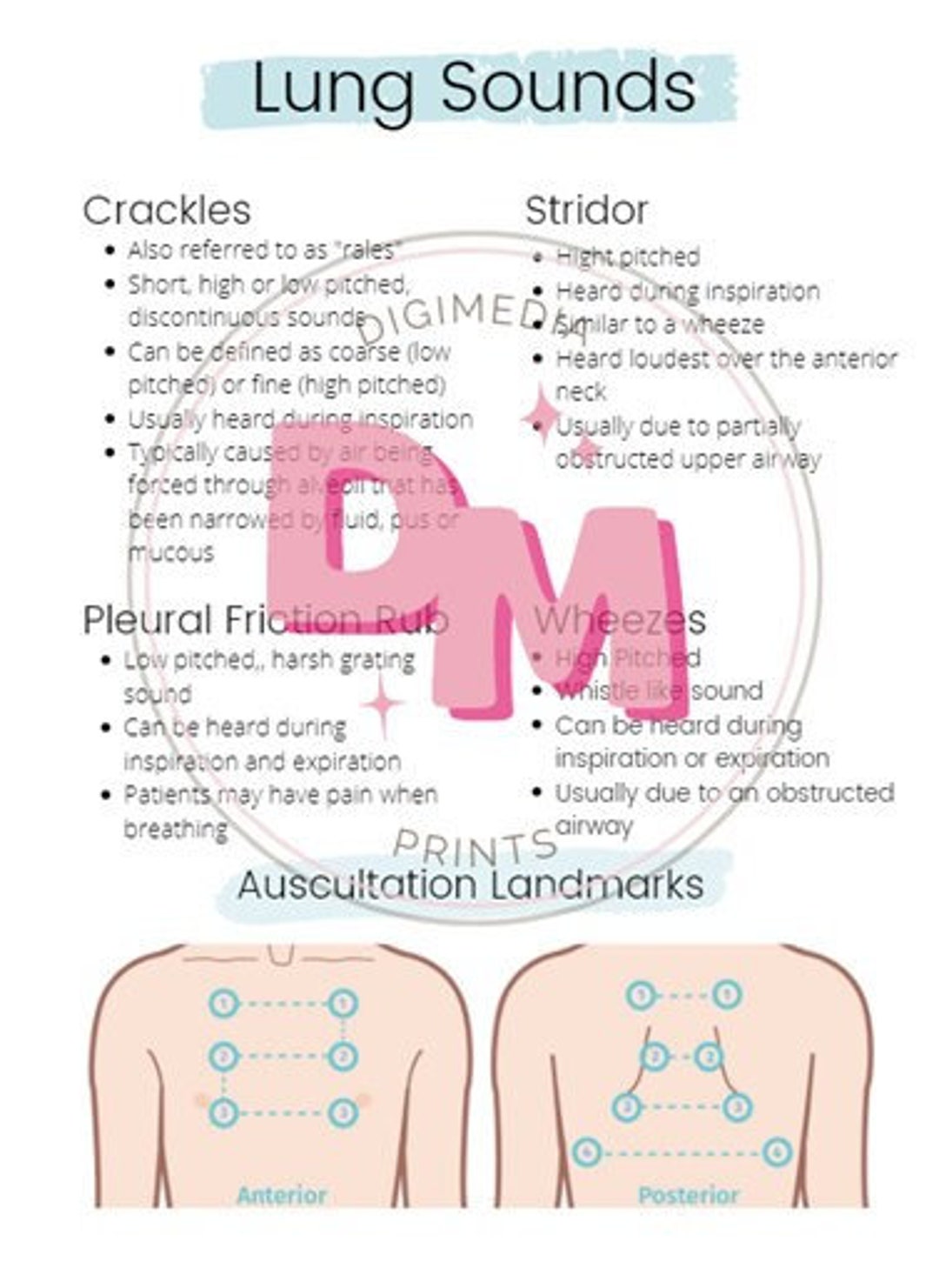
How to Assess Fluid in the Lungs During Auscultation? This article delves into the nuances of identifying fluid in the lungs during auscultation, emphasizing the importance of starting at the lower lung fields to ascertain the presence and extent of fluid accumulation. Auscultation, the process of listening to the sounds produced within the body, is an essential aspect of clinical assessment in respiratory medicine.įluid accumulation in the lungs, a manifestation of conditions like heart failure, pneumonia, or pulmonary edema, can have profound clinical implications.ĭetecting these changes early through auscultation can significantly impact patient outcomes and guide subsequent medical interventions.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
